- Research article
- Open access
- Published:
Systematic literature review assessing tobacco smoke exposure as a risk factor for serious respiratory syncytial virus disease among infants and young children
BMC Pediatrics volume 12, Article number: 81 (2012)
Abstract
Background
The role of environmental tobacco smoke (ETS) exposure as a risk factor for serious respiratory syncytial virus (RSV) disease among infants and young children has not been clearly established. This systematic review was conducted to explore the association between ETS exposure and serious RSV disease in children younger than 5 years, including infants and young children with elevated risk for serious RSV disease.
Methods
A systematic review of English-language studies using the PubMed and EMBASE databases (1990–2009) was performed to retrieve studies that evaluated ETS as a potential risk factor for serious RSV illness. Studies assessing risk factors associated with hospitalization, emergency department visit, or physician visit due to RSV (based on laboratory confirmation of RSV or clinical diagnosis of RSV) in children under the age of 5 years were included.
Results
The literature search identified 30 relevant articles, categorized by laboratory confirmation of RSV infection (n = 14), clinical diagnosis of RSV disease (n = 8), and assessment of RSV disease severity (n = 8). Across these three categories of studies, at least 1 type of ETS exposure was associated with statistically significant increases in risk in multivariate or bivariate analysis, as follows: 12 of 14 studies on risk of hospitalization or ED visit for laboratory-confirmed RSV infection; 6 of 8 studies of RSV disease based on clinical diagnosis; and 5 of the 8 studies assessing severity of RSV as shown by hospitalization rates or degree of hypoxia. Also, 7 of the 30 studies focused on populations of premature infants, and the majority (5 studies) found a significant association between ETS exposure and RSV risk in the multivariate or bivariate analyses.
Conclusion
We found ample evidence that ETS exposure places infants and young children at increased risk of hospitalization for RSV-attributable lower respiratory tract infection and increases the severity of illness among hospitalized children. Additional evidence is needed regarding the association of ETS exposure and outpatient RSV lower respiratory tract illness. Challenges and potential pitfalls of assessing ETS exposure in children are discussed.
Background
Almost all children contract respiratory syncytial virus (RSV) by 2 years of age [1]. RSV causes upper airway infections, bronchiolitis, wheezy bronchitis, and pneumonia. Although most infections produce mild disease, RSV is a major cause of hospitalization in infants [2] and can be fatal [3]. Premature infants, infants with bronchopulmonary dysplasia (BPD) (chronic lung disease of prematurity), and infants with congenital heart disease are at risk for serious infections [4, 5]. Risk factors for RSV infection include exclusive bottle feeding [6, 7], having older brothers or sisters in the household [6, 8, 9], male gender [10], low birth weight [10, 11], prematurity [6], household crowding [12], and young chronologic age [9]. Although exposure to environmental tobacco smoke (ETS) is a risk factor for asthma, wheezing, decreased pulmonary function, otitis media, cough, and lower respiratory tract infections (LRTIs) in general [13], its role in the development of serious RSV disease among infants and young children is less clear and has been a topic of interest among the healthcare community [14].
In this systematic review, we evaluated the evidence of an association between ETS exposure and serious RSV disease among children younger than 5 years. To obtain the broadest understanding of whether ETS exposure affects the risk of serious RSV disease, we placed no limits on the type of proxy measures of ETS exposure. Understanding the evidence basis for ETS exposure and RSV could highlight the need to direct healthcare resources or intervention programs toward this potentially modifiable risk factor.
Methods
Patient population
In this systematic literature review, we included studies of infants and children up to 5 years of age, including studies of children at high risk for serious RSV disease. We defined the high-risk population as patients with prematurity, BPD, or congenital heart disease. All other patient populations were defined as general populations, which consisted predominantly of children not defined as high risk.
Search strategy
Following PRISMA guidelines, we conducted a systematic review of the association of ETS exposure with serious RSV disease by searching broadly for studies assessing various risk factors, including ETS exposure, for RSV, bronchiolitis, or LRTI caused by RSV or bronchiolitis.[15] We searched the PubMed (including MEDLINE) and EMBASE databases for English-language studies published and indexed between 1990 and April 2009. No additional relevant unpublished studies were obtained. Studies that identified ETS exposure as a risk factor might be more likely to mention ETS in the title or abstract than studies that evaluated ETS exposure in a set of other risk factors, but did not find it to be significantly associated with increased risk. To minimize article selection bias across studies, we searched for articles that assessed any risk factors for RSV as well as bronchiolitis, because 50% to 80% of winter bronchiolitis is due to RSV in infants and young children [1]. For PubMed, the National Library of Medicine Medical Subject Headings (MeSH terms) used in the search included tobacco smoke pollution/adverse effects respiratory syncytial virus infections bronchiolitis viral, and respiratory tract infections in combination with the MeSH subheadings epidemiology etiology, and complications. The MeSH heading respiratory tract infections was combined with the keywords syncytial or RSV OR bronchiolitis or the MESH term tobacco smoke pollution/adverse effects. Studies that included risk assessment were identified using the following MeSH headings: analysis of variance (which includes multivariate analysis), probability (which includes proportional hazards model, odds ratio, risk, risk assessment, and risk factors); and case–control studies or cohort studies, which were combined with the terms relative risk OR hazard ratio OR odds ratio. The search identified studies with the following combination of these terms: (1) any disease-related term plus any risk assessment term; or (2) any disease-related term plus the smoke exposure term. We did not search for unpublished studies or reports.
Study selection
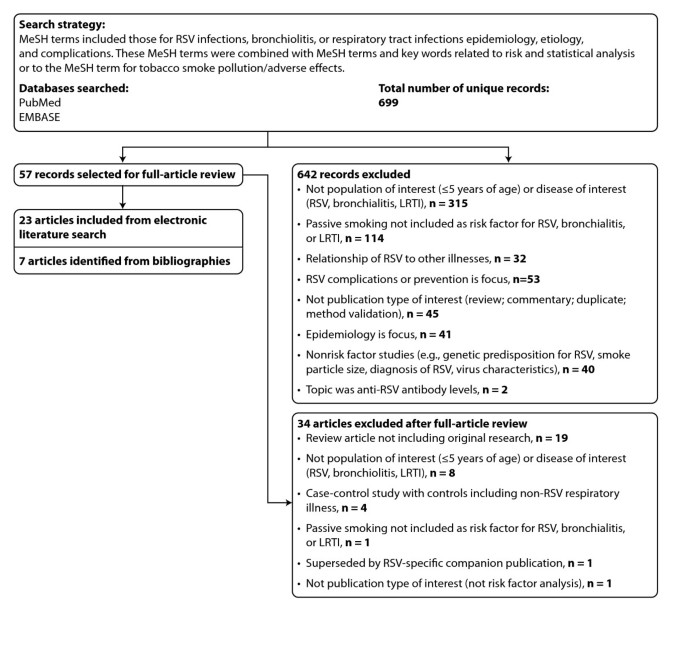
Each relevant article was read by several authors and the bibliographies of included articles were reviewed for additional studies. We excluded studies that did not assess disease risk or did not include ETS exposure as a risk factor. Figure 1 presents a summary of exclusions and rationales for exclusion during successive rounds of review.
PRISMA Flow Diagram: Summary of Exclusions and Rationales for Exclusion During Phases of Systematic Literature Review. PRISMA = Preferred Reporting Items for Systematic Reviews and Meta-Analyses; LRTI = lower respiratory tract infection; MeSH = medical subject headings; RSV = respiratory syncytial virus.
Data extraction
Study details were extracted into tables, and table content was verified by a second author and by a reviewer not involved in the data extraction. The authors discussed each article to reach consensus regarding the study details. For each study the following data were extracted: reference, publication year, country origin, study design, study population size and description, assessment method for ETS exposure (e.g., maternal smoking through birth certificate data), method of ascertainment of RSV status (if any, such as through laboratory confirmation or clinical diagnosis), disease outcome evaluated (e.g., hospitalization for RSV), and results and significance of multivariate, bivariate, and other statistical analyses. Outcomes related to the presence of RSV antibodies without evidence of hospitalization, ED visit, or physician visit related to RSV were not extracted. The principal summary measures were adjusted odds ratios (aORs), adjusted rate ratios (aRRs), or adjusted hazard ratios (aHRs) for multivariate analyses and odds ratios (ORs) for bivariate analyses. Several studies that did not perform multivariate analyses performed between-group comparisons and presented P values.
Assessment of risk of bias
Among the studies meeting the inclusion criteria, we evaluated the risk of bias at the outcome and study level using the Cochrane risk of bias tool [16]. The Cochrane risk of bias tool was developed primarily for use in interventional studies; we used the tool to examine factors specific to sources of bias frequently found in observational studies. The studies were examined for risk of bias that would potentially influence the association of ETS exposure with serious RSV disease. The studies were judged regarding evidence of misclassification bias of RSV disease, selective reporting bias, confounding bias, exposure ascertainment bias, or participant selection bias. Disease misclassification bias was assessed based on the likelihood of the study population having an LRTI that was not due to RSV. We expect that disease misclassification would underestimate the association between ETS exposure and serious RSV disease. Selective reporting bias was evaluated based on whether outcomes related to risk factors were clearly reported. Confounding bias was assessed based on whether the study controlled for the effects of other variables through multivariate analysis. We expect that unadjusted results may overestimate the association between ETS exposure and serious RSV disease. Exposure ascertainment bias was assessed based on whether the ETS exposure variables were described clearly and determined by the study authors to be adequate measures of ETS exposure in the study population. Finally, participant selection bias was pointed out in case–control studies in which the control group consisted of ill patients with non-RSV respiratory disease, and therefore, the effect of ETS exposure on serious RSV disease could be biased toward the null.
Results
The search of PubMed and embase databases yielded 699 unique results, and the abstracts were reviewed for relevance (Figure 1). Of these, 676 were excluded through successive rounds of review, the majority because the studies did not focus on a disease of interest (RSV, bronchiolitis, or LRTI attributable to RSV or bronchiolitis), were not conducted in a population of interest (children younger than 5 years without serious nonrespiratory disease, such as cancer or organ transplant), or did not assess ETS exposure.
Full review of 57 articles resulted in the exclusion of 34 articles, leaving 23 articles identified by the electronic search. The addition of 7 articles identified from references cited (4 were published before 1990) produced a total of 30 relevant articles.
Overview of studies
The results are organized by study characteristics and include a bias assessment summary for each study. (The full bias assessment is presented in Additional file 1: Table S1) Table 1 presents 14 studies that established a diagnosis of RSV disease by confirmatory laboratory testing. These studies compared children with RSV infections with children without respiratory illness and assessed whether ETS exposure increased the risk for developing a serious RSV infection. Table 2 presents 8 studies that did not confirm suspected cases of RSV disease with laboratory testing, but relied on the clinical diagnosis of RSV or bronchiolitis, often from medical charts or insurance data. These studies also compared children with RSV or bronchiolitis infections with children without respiratory illness. Table 3 presents 8 studies that examined the impact of ETS exposure on the severity of RSV disease as measured by hospitalization or degree of hypoxia. These studies started with a sample of children infected with RSV and assessed whether ETS exposure increased the severity of the RSV infection. Within each group of studies, we considered studies of premature infants separately because this population is at higher risk for serious RSV disease than the general population of children [17, 18]. We also present the results by study design (e.g., cohort, case–control) in each table.
The methods used to assess ETS exposure status varied widely and included mother’s prenatal smoking status, mother’s postnatal smoking status, father’s smoking status, smoking in the home, number of smokers in the household, number of cigarettes smoked in the home, more than five cigarettes smoked per day in the home, days of smoke exposure, history of exposure to smoking, smoking by daycare provider, and cotinine levels.
Some of the studies summarized included more than one source of ETS exposure, but no study detailed missing ETS exposure status data. In the studies reporting multiple ETS exposure, we have presented all results based on the different sources (e.g., maternal smoking during pregnancy and smokers in the household) because it is difficult to determine in each setting which of several proxies for total ETS exposure results in the least misclassification error. Few of the multivariate studies provided a rationale for their selection of control variables. We therefore included positive bivariate results in our tables when bivariate and multivariate analyses produced disparate conclusions.
ETS exposure and laboratory-confirmed RSV disease
The studies in Table 1 seek to answer the question, does ETS exposure increase the risk that an uninfected child will develop serious RSV? In 14 studies, the diagnosis of RSV infection was confirmed by laboratory testing (Table 1). Of these, 12 studies showed a significant adverse impact of ETS exposure on serious RSV in bivariate or multivariate analysis as measured by at least one exposure variable. These studies examined the association of ETS exposure and other factors on the risk of ED visit [23] or hospital admission [5, 6, 9, 10, 12, 19–21, 24–26] for laboratory-confirmed RSV LRTI. Two studies examining laboratory-confirmed RSV did not find a statistically significant association between ETS exposure and serious RSV: a cohort study of outpatients in the United States assessing the risk of a child presenting to the pediatrician’s office with an RSV infection [22], and an Australian case–control study assessing the risk of RSV hospitalization [11].
Four of these 14 studies contained at least one significant association, but found mixed results with different ETS exposure variables [6, 19, 20, 23]. One prospective cohort study in premature infants found that maternal smoking and parental smoking in the home had conflicting associations with three different outcomes: RSV LRTI, all-cause hospital admission, and length of hospital stay [19]. Measures of smoke exposure in the home and maternal smoking gave conflicting results when evaluated in 2 studies [6, 20], including a study in premature infants [20]. Finally, a small case–control study in a general population in Turkey found that several exposure variables (only mother smoking, both parents smoking, any parent smoking, and serum cotinine) were associated with significant increase in risk of admittance to the ED; however, only father smoking was significantly associated with a decrease in risk [23].
Of the studies of laboratory-confirmed RSV hospitalization described in Table 1, 5 were conducted in premature infants and 9 were conducted in general populations. All 5 studies of laboratory-confirmed RSV in premature infants found increased risk related to ETS exposure in either bivariate or multivariate analyses [9, 10, 19–21] (Table 1). The 2004 case–control study of infants with a gestational age of 33 to 35 weeks by Figueras-Aloy et al. [21] found an OR of 1.62 in the bivariate analysis that did not remain significant in the multivariate analysis. However, the same researchers published a much larger cohort study in 2008, in a premature population with a gestational age of 32 to 35 weeks, reporting a nearly identical aOR (1.61) for maternal smoking that remained significant in the multivariate analysis [20]. The authors of the 2004 study note that the prevalence of ETS exposure decreased in Spain during the years before the study (52% during the 1999–2000 RSV season compared with 30% in this study) because of anti-smoking campaigns or health education [21]. The significant association in the larger study suggests that the earlier study was underpowered for the multivariate analysis.
Of the 9 studies of laboratory-confirmed RSV illness in general populations described in Tables 1 2 were prospective cohort studies and 7 were case–control studies (Table 1). Risk of RSV LRTI in an outpatient office setting [22] and risk of RSV hospitalization from ETS exposure (smoking in the household, but not from maternal smoking during pregnancy) [6] were not significant in the cohort studies.
The 7 case–control studies of laboratory confirmed RSV illness in general populations ranged in size from 20 to 2,564 cases (Table 1), and all found a significant association between ETS exposure and risk of RSV hospitalization in either the multivariate or bivariate analyses, with the ORs from the 4 largest studies clustering tightly between 1.35 and 1.6. The 3 smallest case–control studies included in Table 1 did not provide ORs but compared ETS exposure prevalence between the cases and healthy controls [23–25]. All 3 found significant differences in ETS exposure in cases versus controls. The Turkish study also demonstrated significantly higher cotinine levels in serum samples from cases than from healthy controls [23]. In a case–control study of Alaska native children, risk was apparent in the bivariate analysis, but not in the multivariate analyses [12] (Table 1). The authors noted that misclassification of exposure status may have been a problem. The study was conducted in Alaska, where children spend much time indoors during the winter RSV season and could be exposed to ETS when visiting other houses or community buildings. This appears likely, because there were smokers living in the households of 59% of the controls and 68% of the cases. The consistency of findings associating ETS exposure and increased risk of serious RSV, coupled with the inconsistency of the variables associated with these significant results, highlights the challenges of assessing and categorizing ETS exposure.
ETS exposure and clinically diagnosed RSV disease
As with the studies in Table 1, the studies in Table 2 seek to answer the question, does ETS exposure increase the risk that an uninfected child will develop serious RSV? In these studies, however, the RSV diagnosis was based on clinical findings rather than a laboratory test. Table 2 presents 8 studies, 6 of which reported a significant association between ETS exposure and bronchiolitis hospitalization or outpatient treatment. Because other organisms may cause bronchiolitis, there may be possible misclassification of RSV disease status [33].
The large general population cohort studies including bronchiolitis hospitalization as an outcome by Boyce et al. [4], Carroll et al. [28], and Koehoorn et al. [29] are in agreement with the 12 studies in Table 1 that identified an increased risk of RSV hospitalization associated with ETS exposure. Carroll and colleagues also demonstrated increased risk of ED visit or clinic visit for bronchiolitis and bronchiolitis diagnosis related to ETS exposure [28].
In other studies assessing risk of bronchiolitis LRTI in children presenting in the office setting, 2 studies found an increased risk for at least one ETS variable [28, 31], whereas 2 other studies did not [29, 30]. Of these, the positive study by Carroll et al. [28] had the greatest statistical power.
Only the Holman study assessed risk of death from bronchiolitis; the risk was increased by maternal smoking (aOR, 1.6) [3].
ETS exposure and severity of RSV illness
The 8 studies in Table 3 address the question, given that a child has contracted RSV, does ETS exposure increase the severity of illness? Four studies compared ETS exposure in children hospitalized for RSV and children with RSV who were not hospitalized. Three of these studies, including a small study of premature infants with BPD, found no effect of ETS exposure on the likelihood of hospitalization for RSV [2, 32, 34]. One small study found an effect of ETS exposure, but only 40% of the hospitalized children were found to have RSV infections, with the remaining 60% representing bronchiolitis caused by other viruses [33].
Four studies examined clinical severity (degree of hypoxemia) of RSV LRTIs among children hospitalized for treatment. All 4 found that ETS exposure was associated with more severe illness (Table 3). Bradley et al. found that hypoxemia was associated with postnatal but not prenatal smoke exposure [36]. Chatzimichael et al. found that breastfeeding was protective against the effect of ETS exposure on disease severity [37]. Based on a small number of studies of RSV severity, ETS exposure does not appear to increase the risk of hospitalization versus outpatient treatment among children infected with RSV, but hospitalized RSV patients exposed to ETS have more severe disease.
Summary of potential bias in observational studies of ETS exposure and serious RSV disease
As the studies reviewed were observational, we evaluated the primary sources of bias that could potentially affect the estimates of association with ETS exposure (Additional file 2). We found that 21 of the 30 studies confirmed the RSV diagnosis through laboratory testing for RSV or multiple respiratory illnesses including RSV in all of the study populations [2, 5, 6, 9–12, 19–26, 32–36, 38]. The remaining studies had a risk of disease misclassification bias of RSV because diagnostic codes (primarily for bronchiolitis) or diagnoses from medical records were used [3, 4, 27–31, 37, 39]. Misclassification of RSV disease may attenuate the association of ETS exposure and severe RSV disease, and the studies of clinically diagnosed RSV patients may provide conservative estimates of ETS exposure risk.
Overall, we identified few studies that had potential selective reporting bias, confounding bias, exposure ascertainment bias for ETS, or participant selection bias. Selective outcome reporting was a potential problem in 2 studies [38, 39], meaning that outcomes were not described sufficiently to determine which factors were included and potentially controlled for in the analysis. Although confounding is a threat across observational studies (because it is difficult to control for both measureable and unmeasurable factors), multivariate analyses were not conducted in a number of studies [23–25, 32, 34, 38], which could lead to an overestimate of the effect of ETS exposure. One study had a high risk of participant selection bias, where both cases and controls were diagnosed with bronchiolitis [33]. Only 2 studies had an unclear risk of ETS exposure [12, 35]. Al-Sonboli and colleagues [35] did not describe how the ETS exposure data or other demographic data were obtained. In the Bulkow et al study, ETS exposure was highly prevalent in the community (in both cases and controls) and indoor visiting was frequent during the winter RSV season [12]; therefore, the ETS exposure variable “smoker in household” was not an adequate proxy for exposure in this population.
No statistical analysis of the risk of bias across studies was performed for this review.
Discussion
The impact of ETS exposure on RSV disease in infants and young children is consistent among studies using laboratory confirmation of RSV infection and clinical diagnosis of bronchiolitis or RSV. Among 14 population-based studies that examined the risk of admission to the hospital or ED for RSV disease, 12 showed that at least one type of ETS exposure in each study was associated with a significant adverse outcome in the bivariate or multivariate analysis. The observation that ETS exposure increases the risk that a child will develop RSV disease that will require hospitalization is robust because these studies used different methods (prospective, retrospective, cohort, case–control) in different patient populations (infants who were premature, term, or with compromising conditions), in a variety of countries and cultures. In addition, the evidence suggests that ETS exposure is associated with more severe hypoxia among children hospitalized for RSV [35–38], and one study found an increased risk of mortality from bronchiolitis [3].
Among studies in premature infants, 5 [9, 10, 19–21] of 7 [9, 10, 19–21, 27, 32] found ETS exposure to be a significant risk factor in bivariate or multivariate analysis, including 5 of the 6 [9, 10, 19–21, 32] studies assessing laboratory-confirmed RSV. One study contradicting this conclusion did not have laboratory confirmation of the diagnosis and relied on a claims database, rather than direct data collection, for ascertainment of the ETS exposure status [27]. Misclassification of disease status or missed diagnosis may have contributed to the negative findings in this study. The other was a small study of 30 premature infants with BPD on home oxygen therapy, 16 of whom developed RSV [32].
The evidence concerning whether ETS exposure increases the risk of mild RSV infection is much less convincing. In a very large study, Carroll et al. found ETS exposure to be associated with only a small increased risk of RSV illness (OR, 1.06) presenting in the outpatient setting [28]. If this OR represents the true risk, the Holberg [22] and Marbury [30] studies, which did not find a risk, would have been underpowered to detect it because of smaller sample sizes. Because nearly all children contract RSV during the first few years of life [1] and most cases are mild [2], there may be a ceiling effect. If children with no ETS exposure are almost certain to contract RSV, ETS exposure can increase the risk of mild infection only slightly.
Misclassification of ETS exposure is a major challenge in studying associations of ETS exposure with disease. Misclassification of exposure status produces a bias in the direction of reducing the apparent magnitude of the risk, leading to either an underestimate of the true ETS exposure risk or to a null finding. Misclassification of an infant or child’s ETS exposure comes from researchers’ use of one or a few measures of possible exposure, which actually can come through many avenues. Examples include in utero exposure through active and passive maternal smoking and postnatal smoking by the mother, father, other individuals living in the home, visitors, and babysitters. ETS exposure outside the home occurs in public places, day care settings, and houses of friends and relatives. No study in this review gathered exposure data for all potential sources. The smoking status of, for example, the parent is a poor proxy for this global exposure as demonstrated by cotinine level studies. Urinary or serum cotinine (a metabolite of nicotine) is an objective measure of ETS exposure but provides information regarding only the previous 48 to 72 hours of exposure [40]. In one study, infants whose parents reported that they did not smoke had mean cotinine levels that were 80% as high as those for infants with one smoking parent [39]. Some infants of nonsmoking parents had higher cotinine levels than some infants with two smoking parents [39].
Confounding bias is another potential obstacle to determining the association between ETS exposure and serious RSV disease. A few studies found an ETS exposure effect in bivariate analyses but not in multivariate analyses after adjustment for other factors [11, 21, 39]. Multivariate models that include ETS exposure and its related factors may be difficult to interpret due to potential collinearity. Smoking status has a well-known association with socioeconomic status (SES) [41], and SES is predictive of ETS exposure in children [42]. Therefore, SES may be a proxy for global ETS exposure over the early years of life. In addition to SES, smoking status is also predicted by race, educational attainment, and marital status [43]. Few of the multivariate studies provided a rationale for their selection of control variables. In reporting of future studies, greater details about the multivariate modeling steps may aid in assessment of collinearity when significant bivariate outcomes become nonsignificant in multivariate analysis.
This review has several limitations. The search was limited to studies published from 1990 to April 2009 in the English language. We searched only Pubmed and Embase and did not attempt to locate unpublished studies. The nature of the primary studies precluded a meta-analysis. The large retrospective database analyses included in this study (Table 2) all depended on bronchiolitis or RSV disease classification from diagnostic codes or medical record diagnosis. Although RSV is a leading cause of LRTI in infants and children, identifying the etiology of LRTI is not systematically undertaken in EDs or physician offices. Methods and reporting of ETS exposure ascertainment in these studies also varies widely. However, in most studies, data on the child’s ETS exposure level ultimately are gathered from parent or caregiver report, whether through direct data collection for the study or, for example, through retrospective review of the mother’s prenatal health records. Our review highlights the inherent difficulty of accurately assessing global ETS exposure.
Conclusion
Overall we found ample evidence that ETS exposure places infants and young children at increased risk of hospitalization for RSV-attributable LRTIs, and increases the severity of illness as measured by degree of hypoxia among children hospitalized for RSV. Based on a small number of studies, we also found evidence that ETS exposure does not increase the likelihood among general populations with RSV of hospitalization versus outpatient treatment.
The prevention of serious RSV illness provides one more rationale for protecting infants and young children from exposure to tobacco smoke, especially high-risk groups such as premature infants and those with chronic conditions who are considered at increased risk of serious RSV disease.
References
Hall CB: Textbook of Pediatric Infectious Diseases. 1998, WB Saunders, Philadelphia, PA, 2084-2110. 4
Hall CB, Weinberg GA, Iwane MK, Blumkin AK, Edwards KM, Staat MA, Auinger P, Griffin MR, Poehling KA, Erdman D, et al: The burden of respiratory syncytial virus infection in young children. N Engl J Med. 2009, 360 (6): 588-598. 10.1056/NEJMoa0804877.
Holman RC, Shay DK, Curns AT, Lingappa JR, Anderson LJ: Risk factors for bronchiolitis-associated deaths among infants in the United States. Pediatr Infect Dis J. 2003, 22 (6): 483-490.
Boyce TG, Mellen BG, Mitchel EF, Wright PF, Griffin MR: Rates of hospitalization for respiratory syncytial virus infection among children in Medicaid. J Pediatr. 2000, 137 (6): 865-870. 10.1067/mpd.2000.110531.
Nielsen HE, Siersma V, Andersen S, Gahrn-Hansen B, Mordhorst CH, Norgaard-Pedersen B, Roder B, Sorensen TL, Temme R, Vestergaard BF: Respiratory syncytial virus infection—risk factors for hospital admission: a case–control study. Acta Paediatr. 2003, 92 (11): 1314-1321. 10.1080/08035250310006304.
von Linstow ML, Hogh M, Nordbo SA, Eugen-Olsen J, Koch A, Hogh B: A community study of clinical traits and risk factors for human metapneumovirus and respiratory syncytial virus infection during the first year of life. Eur J Pediatr. 2008, 167 (10): 1125-1133. 10.1007/s00431-007-0643-4.
Nafstad P, Jaakkola JJ, Hagen JA, Botten G, Kongerud J: Breastfeeding, maternal smoking and lower respiratory tract infections. Eur Respir J. 1996, 9 (12): 2623-2629. 10.1183/09031936.96.09122623.
Carbonell-Estrany X, Quero J, Bustos G, Cotero A, Domenech E, Figueras-Aloy J, Fraga JM, Garcia LG, Garcia-Alix A, Del Rio MG, et al: Rehospitalization because of respiratory syncytial virus infection in premature infants younger than 33 weeks of gestation: a prospective study. IRIS Study Group. Pediatr Infect Dis J. 2000, 19 (7): 592-597. 10.1097/00006454-200007000-00002.
Carbonell-Estrany X, Quero J: Hospitalization rates for respiratory syncytial virus infection in premature infants born during two consecutive seasons. Pediatr Infect Dis J. 2001, 20 (9): 874-879. 10.1097/00006454-200109000-00010.
Law BJ, Langley JM, Allen U, Paes B, Lee DS, Mitchell I, Sampalis J, Walti H, Robinson J, O'Brien K, et al: The Pediatric Investigators Collaborative Network on Infections in Canada study of predictors of hospitalization for respiratory syncytial virus infection for infants born at 33 through 35 completed weeks of gestation. Pediatr Infect Dis J. 2004, 23 (9): 806-814. 10.1097/01.inf.0000137568.71589.bd.
Reeve CA, Whitehall JS, Buettner PG, Norton R, Reeve DM, Francis F: Predicting respiratory syncytial virus hospitalisation in Australian children. J Paediatr Child Health. 2006, 42 (5): 248-252. 10.1111/j.1440-1754.2006.00849.x.
Bulkow LR, Singleton RJ, Karron RA, Harrison LH, Alaska RSVSG: Risk factors for severe respiratory syncytial virus infection among Alaska native children. Pediatrics. 2002, 109 (2): 210-216. 10.1542/peds.109.2.210.
Office of Health and Environmental Assessment: Respiratory health effects of passive smoking: lung cancer and other disorders (EPA/600/6-90/006F). 1992, US Environmental Protection Agency, Washington, DC
Committee on Infectious Diseases: From the American Academy of Pediatrics: Policy statements–Modified recommendations for use of palivizumab for prevention of respiratory syncytial virus infections. Pediatrics. 2009, 124 (6): 1694-1701.
Moher D, Liberati A, Tetzlaff J, Altman DG: Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. PLoS Med. 2009, 6 (7): e1000097-10.1371/journal.pmed.1000097.
The Cochrane Collaboration’s tool for assessing risk of bias. http://www.ohg.cochrane.org/forms/Risk%20of%20bias%20assessment%20tool.pdf,
The IMpact-RSV Study Group: Palivizumab, a humanized respiratory syncytial virus monoclonal antibody, reduces hospitalization from respiratory syncytial virus infection in high-risk infants. Pediatrics. 1998, 102 (3 Pt 1): 531-537.
Horn SD, Smout RJ: Effect of prematurity on respiratory syncytial virus hospital resource use and outcomes. J Pediatr. 2003, 143 (5 suppl): S133-S141.
Broughton S, Roberts A, Fox G, Pollina E, Zuckerman M, Chaudhry S, Greenough A: Prospective study of healthcare utilisation and respiratory morbidity due to RSV infection in prematurely born infants. Thorax. 2005, 60 (12): 1039-1044. 10.1136/thx.2004.037853.
Figueras-Aloy J, Carbonell-Estrany X, Quero-Jimenez J, Fernandez-Colomer B, Guzman-Cabanas J, Echaniz-Urcelay I, Domenech-Martinez E: FLIP-2 Study: risk factors linked to respiratory syncytial virus infection requiring hospitalization in premature infants born in Spain at a gestational age of 32 to 35 weeks. Pediatr Infect Dis J. 2008, 27 (9): 788-793. 10.1097/INF.0b013e3181710990.
Figueras-Aloy J, Carbonell-Estrany X, Quero J: Case–control study of the risk factors linked to respiratory syncytial virus infection requiring hospitalization in premature infants born at a gestational age of 33–35 weeks in Spain. Pediatr Infect Dis J. 2004, 23 (9): 815-820. 10.1097/01.inf.0000136869.21397.6b.
Holberg CJ, Wright AL, Martinez FD, Ray CG, Taussig LM, Lebowitz MD: Risk factors for respiratory syncytial virus-associated lower respiratory illnesses in the first year of life. Am J Epidemiol. 1991, 133 (11): 1135-1151.
Gurkan F, Kiral A, Dagli E, Karakoc F: The effect of passive smoking on the development of respiratory syncytial virus bronchiolitis. Eur J Epidemiol. 2000, 16 (5): 465-468. 10.1023/A:1007658411953.
Hall CB, Hall WJ, Gala CL, MaGill FB, Leddy JP: Long-term prospective study in children after respiratory syncytial virus infection. J Pediatr. 1984, 105 (3): 358-364. 10.1016/S0022-3476(84)80005-0.
Hayes EB, Hurwitz ES, Schonberger LB, Anderson LJ: Respiratory syncytial virus outbreak on American Samoa. Evaluation of risk factors. Am J Dis Child. 1989, 143 (3): 316-321.
Stensballe LG, Kristensen K, Simoes EA, Jensen H, Nielsen J, Benn CS, Aaby P: Atopic disposition, wheezing, and subsequent respiratory syncytial virus hospitalization in Danish children younger than 18 months: a nested case–control study. Pediatrics. 2006, 118 (5): e1360-e1368. 10.1542/peds.2006-0907.
Gavin NI, Leader S: Predictive accuracy of risk factors for RSV-related hospitalizations among infants in low-income families born at 32 to 35 weeks of gestation. J Clin Outcomes Manag. 2007, 14 (6): 323-331.
Carroll KN, Gebretsadik T, Griffin MR, Dupont WD, Mitchel EF, Wu P, Enriquez R, Hartert TV: Maternal asthma and maternal smoking are associated with increased risk of bronchiolitis during infancy. Pediatrics. 2007, 119 (6): 1104-1112. 10.1542/peds.2006-2837.
Koehoorn M, Karr CJ, Demers PA, Lencar C, Tamburic L, Brauer M: Descriptive epidemiological features of bronchiolitis in a population-based cohort. Pediatrics. 2008, 122 (6): 1196-1203. 10.1542/peds.2007-2231.
Marbury MC, Maldonado G, Waller L: The indoor air and children's health study: methods and incidence rates. Epidemiology. 1996, 7 (2): 166-174. 10.1097/00001648-199603000-00011.
McConnochie KM, Roghmann KJ: Parental smoking, presence of older siblings, and family history of asthma increase risk of bronchiolitis. Am J Dis Child. 1986, 140 (8): 806-812.
Groothuis JR, Gutierrez KM, Lauer BA: Respiratory syncytial virus infection in children with bronchopulmonary dysplasia. Pediatrics. 1988, 82 (2): 199-203.
Al-Shehri MA, Sadeq A, Quli K: Bronchiolitis in Abha, Southwest Saudi Arabia: viral etiology and predictors for hospital admission. West Afr J Med. 2005, 24 (4): 299-304.
Somech R, Tal G, Gilad E, Mandelberg A, Tal A, Dalal I: Epidemiologic, socioeconomic, and clinical factors associated with severity of respiratory syncytial virus infection in previously healthy infants. Clin Pediatr (Phila). 2006, 45 (7): 621-627. 10.1177/0009922806291012.
Al-Sonboli N, Hart CA, Al-Aghbari N, Al-Ansi A, Ashoor O, Cuevas LE: Human metapneumovirus and respiratory syncytial virus disease in children, Yemen. Emerg Infect Dis. 2006, 12 (9): 1437-1439.
Bradley JP, Bacharier LB, Bonfiglio J, Schechtman KB, Strunk R, Storch G, Castro M: Severity of respiratory syncytial virus bronchiolitis is affected by cigarette smoke exposure and atopy. Pediatrics. 2005, 115 (1): e7-e14.
Chatzimichael A, Tsalkidis A, Cassimos D, Gardikis S, Tripsianis G, Deftereos S, Ktenidou-Kartali S, Tsanakas I: The role of breastfeeding and passive smoking on the development of severe bronchiolitis in infants. Minerva Pediatr. 2007, 59 (3): 199-206.
Sritippayawan S, Prapphal N, Wong P, Tosukhowong P, Samransamruajkit R, Deerojanawong J: Environmental tobacco smoke exposure and respiratory syncytial virus infection in young children hospitalized with acute lower respiratory tract infection. J Med Assoc Thai. 2006, 89 (12): 2097-2103.
Reese AC, James IR, Landau LI, Lesouef PN: Relationship between urinary cotinine level and diagnosis in children admitted to hospital. Am Rev Respir Dis. 1992, 146 (1): 66-70.
Benowitz NL, Jacob P: Nicotine and cotinine elimination pharmacokinetics in smokers and nonsmokers. Clin Pharmacol Ther. 1993, 53 (3): 316-323. 10.1038/clpt.1993.27.
Tobacco use among U.S. racial/ethnic minority groups—African Americans, American Indians and Alaska Natives, Asian Americans and Pacific Islanders, Hispanics. A Report of the Surgeon General. Executive summary. MMWR Recomm Rep. 1998, 47 (RR-18): v-xv. 1–16
Windham GC, Swan SH, Fenster L: Parental cigarette smoking and the risk of spontaneous abortion. Am J Epidemiol. 1992, 135 (12): 1394-1403.
Office of the Surgeon General: The health consequences of smoking: a report of the Surgeon General. Edited by Services UDoHaH. Washington, DC. 2004, US Department of Health and Human Services
Pre-publication history
The pre-publication history for this paper can be accessed here:http://www.biomedcentral.com/1471-2431/12/81/prepub
Acknowledgements
Editorial assistance was provided by Susan DeRocco, PhD, and Gerard P. Johnson, PhD, of Complete Healthcare Communications, Inc. (Chadds Ford, PA) and was funded by MedImmune.
Author information
Authors and Affiliations
Corresponding author
Additional information
Competing interests
This project was funded under a contract with MedImmune, LLC. Joseph R. DiFranza, MD, provided consultant services to MedImmune. Amy M. Barrett, MSPH, MA, and Ann D. Colosia, PhD, are employees of RTI Health Solutions and provided consulting services to MedImmune. Parthiv J. Mahadevia, MD, MPH, and Anthony Masaquel, PhD, MPH, are employees of MedImmune. All authors agreed on the final text and conclusions of the manuscript. There are no other competing interest disclosures.
Authors’ contributions
JD participated in the conception of the literature review and paper, reviewed published studies, analyzed data, and drafted portions of the manuscript. AM participated in the conception of the literature review and paper, reviewed studies, analyzed data, and critically revised the manuscript for important intellectual content. AB and AC each participated in the design and conception of the literature review and paper, reviewed published studies, extracted and analyzed data, and drafted portions of the manuscript. PM participated in the conception of the manuscript, analyzed data, and critically revised the manuscript for important intellectual content. All authors read and approved the final manuscript.
Electronic supplementary material
12887_2011_593_MOESM1_ESM.pdf
Additional file 1: Table S1. Provides full bias assessment of studies reported in this systematic literature review. (PDF 198 KB)
Authors’ original submitted files for images
Below are the links to the authors’ original submitted files for images.
Rights and permissions
This article is published under license to BioMed Central Ltd. This is an Open Access article distributed under the terms of the Creative Commons Attribution License (http://creativecommons.org/licenses/by/2.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
About this article
Cite this article
DiFranza, J.R., Masaquel, A., Barrett, A.M. et al. Systematic literature review assessing tobacco smoke exposure as a risk factor for serious respiratory syncytial virus disease among infants and young children. BMC Pediatr 12, 81 (2012). https://doi.org/10.1186/1471-2431-12-81
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/1471-2431-12-81